Did you know that chronic venous hypertension is prevalent in 25-40% of women and 10-20% of men? This chronic illness is too common to ignore.
Understanding chronic venous hypertension can be complicated. As with most bodily diseases, there are many interwoven factors that may make understanding illnesses more difficult. However, we’re here to help if you’re looking to learn more about this chronic illness.
To learn more about what chronic venous hypertension is, how it’s caused, and how you can prevent it, keep reading. We have everything you need to know.
How Do the Veins in Our Legs Work?
In order to properly address chronic venous hypertension, we first have to cover how the veins in our legs work.
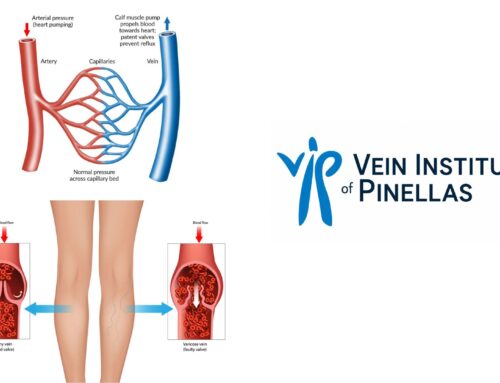
Veins carry blood towards the heart. Because of this process, veins flow at a lower pressure than arteries (which carry blood away from the heart).
The entire venous system is made up of different ‘levels’ of veins. There are deep veins and superficial veins that are joined by perforator veins.
All of the veins in our legs have valves that help the blood travel from the superficial veins to the deep veins so that it can make its way back to the heart. This blood travels via the perforators.
These valves are extremely important given that the blood has to be pumped a long distance to the heart. This is made even more important if you’re standing and your blood is being pulled down by gravity.
If your venous valves aren’t working correctly, this could cause the blood to flush back out into the superficial veins. This leads to increased pressure in those veins. This is referred to as chronic venous hypertension.
What Is Chronic Venous Hypertension?
The venous valves in your legs can become damaged by a multitude of things: pregnancy, obesity, surgery, trauma, and more. If your valves do become damaged, this causes the backflow (reflux) of blood back into the superficial veins via the perforators as we discussed.
As the blood refluxes, it starts to accumulate in the lower leg. As the volume rises, the pressure rises. Hence, this condition is called chronic venous hypertension.
Even worse, the blood will continuously accumulate and cause the valves themselves to stretch. The more that the valves stretch, the more unlikely it is that they will be able to close. Some valves become stuck in this open position.
Broken valves only cause even more of an issue for those who have this condition. Since the blood is no longer being led into the deep veins, it will continue to build up even more volume and pressure.
Valves can also become damaged by a build-up of fibrous tissue. After someone receives treatment for a blood clot, they may not actually heal completely. The remaining residue could become fibrous.
As the fibrous tissue builds and builds, it becomes an obstruction in the vein in which it is located. If that fibrous tissue builds in the venous valve, this could cause the valve to become tangled up in the fibrous tissue. Needless to say, this could cause the valve to build more pressure in the leg.
What Are the Signs of Chronic Venous Hypertension?
There are a few physical signs that come with chronic venous hypertension. If you’re afraid that you may have chronic venous hypertension, you should look out for these.
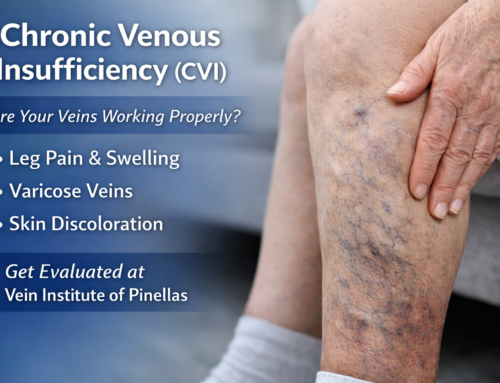
You should be more concerned about developing chronic venous hypertension if you experience pain, swelling, heaviness, and discomfort in your lower legs.
Ankle flare. Chronic venous hypertension can cause the capillaries in the ankle to swell. This leads to visible changes, especially on the inner ankle.
Varicose veins. Veins can become visible on the lower legs as they’re stretched by the amount of blood that is accumulating in the veins. This can cause itching and pain as the veins hold more and more blood.
Oedema. As blood builds up, it can spill over into the tissues. This can cause pain, discomfort, and swelling.
Varicose eczema. Chronic venous hypertension can lead to dry, flaky skin with weeping. This condition is also marked by an increase in skin sensitivity and dryness.
Lipodermatosclerosis. This condition can cause your leg to become hard like wood due to inflammation. It also leads to dryness.
Haemosiderin staining. The leakage of blood from the veins can cause the tissue to turn a rust-brown color. People with this condition may be able to see the staining on their inner ankle.
What Are the Risk Factors for Chronic Venous Hypertension?
Chronic venous hypertension is affected by many conditions and qualities.
As you may have noticed at the beginning of this post, women are more likely to have chronic venous hypertension. Along with this, those who do a lot of heavy lifting or do a lot of standing (whether for their job or otherwise) are more likely to develop chronic venous hypertension.
We also mentioned that chronic venous hypertension is more common among those who are overweight or obese. Varicose veins are common among pregnant women, especially during the early part of their first pregnancy. Scientists are not entirely sure as to why since women do not gain that much weight in early pregnancy, but research is being done on this topic.
There may also be a link between chronic venous hypertension and smoking. The link between these two may especially be true for males.
What About the Link Between Leg Ulcerations and Chronic Venous Hypertension?
No one understands the link between leg ulcerations and chronic venous hypertension completely. However, whatever the link is, it remains strong.
Some theories believe that the blood building up in the veins and spreading to the surrounding capillaries and tissues may cause leg ulcers to form. It is also believed that the blood build-up may be what causes the slow healing when it comes to leg ulcers.
One theory, known as the fibrin cuff theory, suggests that the blood builds up and creates a barrier. Within this barrier, blood continues to build up. This includes white blood cells.
These white blood cells are stuck in this region and unable to heal the damage that may have been done to the skin. Hence, ulceration may occur and heal very slowly.
Another theory speaks towards growth factors becoming trapped in the dermis (a layer of the skin).
No matter what theory scientists gather around, the link still remains true. It is definitely complex in its arrangement and development.
What Do I Do If I Think I Have Chronic Venous Hypertension?
If you feel like you may be experiencing chronic venous hypertension, you should talk to your physician. Your doctor may conduct a physical examination of your legs to see if there are any swelling and/or tenderness.
In addition, your doctor may perform a duplex ultrasound or a venogram.
A duplex ultrasound helps the physician view blood flow through your legs. They can see if there is any backflow or other blood accumulation in your legs.
A venogram uses IV contrast and a series of x-rays to view how blood goes through your venous valves and throughout your body. The IV contrast appears opaque on the x-ray films. This allows the physician to see clearly where your blood vessels are and how the blood is moving.
Your physician may or may not be able to determine your condition without using either the ultrasound or the x-ray. Your severity may be physically recognizable.
How Do I Manage Chronic Venous Hypertension?
Managing chronic diseases can be a difficult task. Managing chronic venous hypertension is no different.
The number one treatment for chronic venous hypertension is compression. If you’ve ever heard of compression socks, you already know what we’re talking about.
Surprisingly, compression helps with solving some of the problems related to chronic venous hypertension. It helps correct valve closure and reduces reflux.
Compression speeds up blood flow and reduces the amount of blood that stays built up in your lower legs. It also helps reduce dryness and improve the overall appearance of the skin.
Exercise also helps improve the effects of chronic venous hypertension. Because exercise gets you moving, it helps increase blood flow.
Elevating the legs also assists in reducing the swelling and pain that comes with chronic venous hypertension. Just as gravity causes blood to build up when you’re standing, it also helps blood flow back to your heart when your legs are elevated.
If the condition is severe, the individual may need to consider vein surgery to correct the venous valves and improve blood flow.
Where Can I Get My Chronic Venous Hypertension Treated?
There are many physicians and vein institutes that can help you control and treat your chronic venous hypertension. However, the Vein Institute of Pinellas is renowned as the number one rated vein treatment expert in the Bay Area. We’re also located in St. Petersburg and Sun City Center.
We treat varicose veins, spider veins, and more with a variety of treatment options.
Contact us today to get an appointment with one of our vein experts. We’ll be happy to discuss your diagnosis and treatment options.



Leave A Comment